Immune-Mediated Thrombocytopenia (ITP) in Dogs
By Professor Michael Herrtage, James Warland, Andrew Kent & Julien Bazelle
The Queen's Veterinary School Hospital, University of Cambridge
Thrombocytes, or platelets, are the body's first defence against bleeding. They are tiny fragments of cells in the blood stream that are produced by the bone marrow. These fragments constantly patrol all of the vessels of the body in order to form a clot if any damage is caused to the vessel wall. In order to function normally, there are usually over 175,000,000 platelets in every millilitre of your dog's blood (up to 500,000,000/ml). The platelets form the first part of clot formation, but other factors are necessary to form an adequate clot if any damage occurs to the blood vessel.
If there are insufficient numbers of platelets present, the blood is not able to quickly form a normal clot. In a condition called immune mediated thrombocytopenia, the dog's own immune system attacks and destroys these platelets.
Although in most cases, thrombocytopenia is the only problem, in some cases ITP will be part of a wider autoimmune condition, with other organs affected. Examples of this include Evan's Syndrome, where the body attacks both the platelets and red blood cells (causing anaemia) or Systemic Lupus Erythematosus (SLE), where the body attacks multiple tissues.
Causes and Diagnostic Tests
ITP is caused by an autoimmune attack against the dog's own platelets, and usually the initial cause of this is unknown. It can be a primary problem or a secondary problem, triggered by other diseases. In the case of a dog with abnormal bleeding, your vet will need to run some tests to establish the cause. Blood tests will show a low platelet count (thrombocytopenia), however, it should be noted that ITP is not the only cause of thrombocytopenia.
Depending on your dog's previous medical history and their findings, your vet may choose to do further tests to look for an underlying cause of the thrombocytopenia. ITP can be caused by various infections, including viral and bacterial infections. The most important type of infection to cause thrombocytopenia in the UK is Ehrlichia, which is spread by ticks, and your vet will be able to test for this if infection is possible. Your vet may also perform other tests, such as X-rays and ultrasound of your dog to look for other causes of thrombocytopenia. Some drug treatments, particularly antibiotics and anti-inflammatory drugs, can cause thrombocytopenia. Unfortunately, ITP is diagnosed by ruling out other potential causes of low platelet numbers.
It is important to inform your vet if your dog has travelled outside the UK, as various infections that are not native to the UK can cause thrombocytopenia and it may be appropriate to test for these as well.
Clinical Signs
In dogs with ITP the most common clinical signs are associated with bleeding. Because clots are constantly being formed to prevent bleeding, even when no obvious trauma has occurred, dogs usually show signs of bleeding even without injuring themselves. Nosebleeds, bruising of the skin or gums, or petechiae (small red spotted rash caused by leaking capillaries) are common signs of ITP. Some dogs will have bleeding into their intestines, which cannot be seen initially, but leads to black, tar-like faeces (melaena). Some dogs will have more unusual sites of bleeding that can lead to other problems, such as bleeding in the brain or the eye.
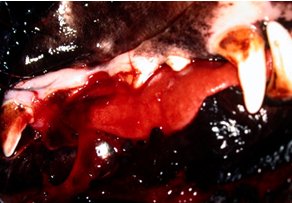 Bleeding from the gums in an Irish Wolfhound with ITP |
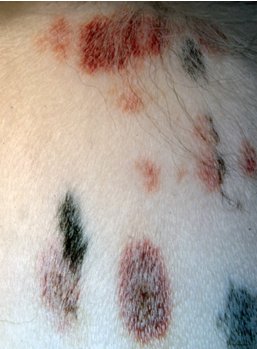 Small petechial haemorrhages in the skin of a Springer Spaniel with ITP |
ITP Bruising on a Dachshund / Basset |
Treatment
In ITP, the treatment is first aimed at decreasing the overactive immune system which causes this platelet reduction. The drugs used to decrease the overactivity of the immune system are called immunosuppressive drugs.
The main type of immunosuppressive drugs is corticosteroids, of which prednisolone remains the most frequently prescribed. Doses of prednisolone vary markedly between patients but high doses are generally used at the beginning of the treatment. Like any medication, prednisolone can be associated with side effects (e.g. increased drinking and urination, increased appetite, weakness, or rarely vomiting or diarrhoea). These side effects are by far less frequent than in human patients, allowing some canine patients to be treated only with prednisolone for a prolonged period.
If prednisolone alone does not control the clinical signs or if side effects are noticed, your own vet may also prescribe other immunosuppressive drugs (e.g. azathioprine, cyclosporine).
If the platelets level is critically low and bleeding had occurred, your veterinarian may suggest transfusion of fresh canine blood or other blood components. As in human patients, transfusion reactions may occur and your dog will have to be closely monitored during this transfusion. In dogs, transfusion reactions are rare after the first transfusion. However, if your dog has already received a blood transfusion, the risk for adverse reactions increases markedly. It is important to mention previous transfusions to your own veterinarian.
The spleen is the principal site of destruction of platelets during ITP. A surgery to remove the spleen has been advocated in severe cases of ITP which failed to respond to medical treatment. We rarely recommend this surgery in our hospital but this must be discussed with your own veterinarian.
If ITP is severe enough, hospitalisation in a referral hospital may be needed. In a referral hospital access to unusual medications, including human medication may be facilitated (e.g. intravenous human immunoglobulin, vincristine, mycophenolate mofetil).
Risks
ITP is considered to be idiopathic or primary when no underlying cause is found. Secondary ITP occurs when an underlying cause is identified which may include:
" Rickettsial infections e.g. Ehrlichia canis, Anaplasma phagocytophilum
" Drugs e.g. trimethoprim/sulfadiazine, cephalosporin
" Cancers
Any breed, sex or age of dog can be affected by ITP. It seems to be more common in middle aged, female dogs, particularly Cocker Spaniels, Old English Sheepdogs, Miniature and Toy Poodles.
People often worry that the ITP has been triggered by recent vaccination, as this link has been established in humans (although is exceedingly rare). In dogs it has not been proven that any vaccination causes ITP, and if it does occur it is also likely to be a rare event. It is very important to remember that many of the diseases your dog is vaccinated against are far more dangerous and common than the rare side effects associated with vaccination. If you are concerned about side effects of vaccination in dogs please discuss this with your veterinarian.
Prevalence
In a study of dogs in the USA, 5.2% of dogs admitted to a specialist veterinary hospital were found to have reduced numbers of platelets. Of these dogs 5% were diagnosed with ITP meaning it was the cause of 0.26% of hospital admissions.
This suggests that it is still a fairly uncommon disease, however it was the most likely cause of developing a very low platelet count (< 36,000,000 platelets/ml).
Outlook
The majority (>70%) of dogs with IMT (Immune-Mediated Thrombocytopenia) will show significant improvement with prednisolone alone or in combination with other immunosuppressive drugs in less than a week. After stabilisation with treatment, the doses are usually slowly tapered down while monitoring closely the platelet value.
During this progressive reduction in dose, there is a risk of recurrence of the clinical signs which may be observed in around 25% of the patients. Following recurrence, treatment should be reinstituted at a higher dosage and your veterinarian will discuss further treatment options.
Unfortunately, despite appropriate treatment around 10 to 15% of dogs with ITP can die or are euthanised at the beginning of the disease or after recurrence of their signs. This is mainly observed with severe disease associated with complications like coagulation disorders or severe gastro-intestinal bleeding. Rapid institution of the treatment and close monitoring during hospitalisation have been associated with reduced risk in dogs with ITP.
If you are owned by a dog or other pet with ITP and wish to use the services of the ITP Support Association, do feel free to join our Association or make a donation to help us with our work. There is no state funding for ITP research, and this charity cannot fund ITP research without help from those who have an interest in finding a cure, whether it be patient, family member, friend or pet owner.
Association's Veterinary Advisor
Andrew Kent BVSc DipECVIM-CA MRCVS
European Veterinary Specialist in Small Animal Internal Medicine
Willows Referral Service
Highlands Road
Shirley
Solihull
West Midlands B90 4NH
United Kingdom
www.willows.uk.net/specialist-services
References:
- Botsch V., Hüchenhoff H., Hartman K. and Hirschberger J., "Retrospective study of 871 dogs with thrombocytopenia." Veterinary Record. 2009; 164, May, 23, 647-651.
- Grindem C.B., Breitschwerdt E.B., Corbett W.T., Jans H.E., "Epidemiologic survey of thrombocytopaenia in dogs: A report on 987 cases." Veterinary Clinical Pathology 1991; 20: 38-43.
- Huang A.A., Moore G.E., and Scott-Moncrieff J.C., "Idiopathic Immune-Mediated Thrombocytopenia and Recent Vaccination in Dogs," Journal of Veterinary Internal Medicine 26, No. 1, 142-148.
- Laurel J. and Gershwin D.V.M., "Autoimmune Diseases in Small Animals," Veterinary Clinics of NA: Small Animal Practice 40, No. 3: 439-457.
- O'Marra S.K., Delaforcade A.M., and Shaw S.P., "Treatment and Predictors of Outcome in Dogs with Immune-Mediated Thrombocytopenia." Journal of the American Veterinary Medical Association 238, No. 3: 346-352.
- Putsche J.C., Kohn B., "Primary immune-mediated thrombocytopenia in 30 dogs (1997-2003)." Journal of the American Animal Hospital Association, 2008, 44, 250-257.
